Blogs
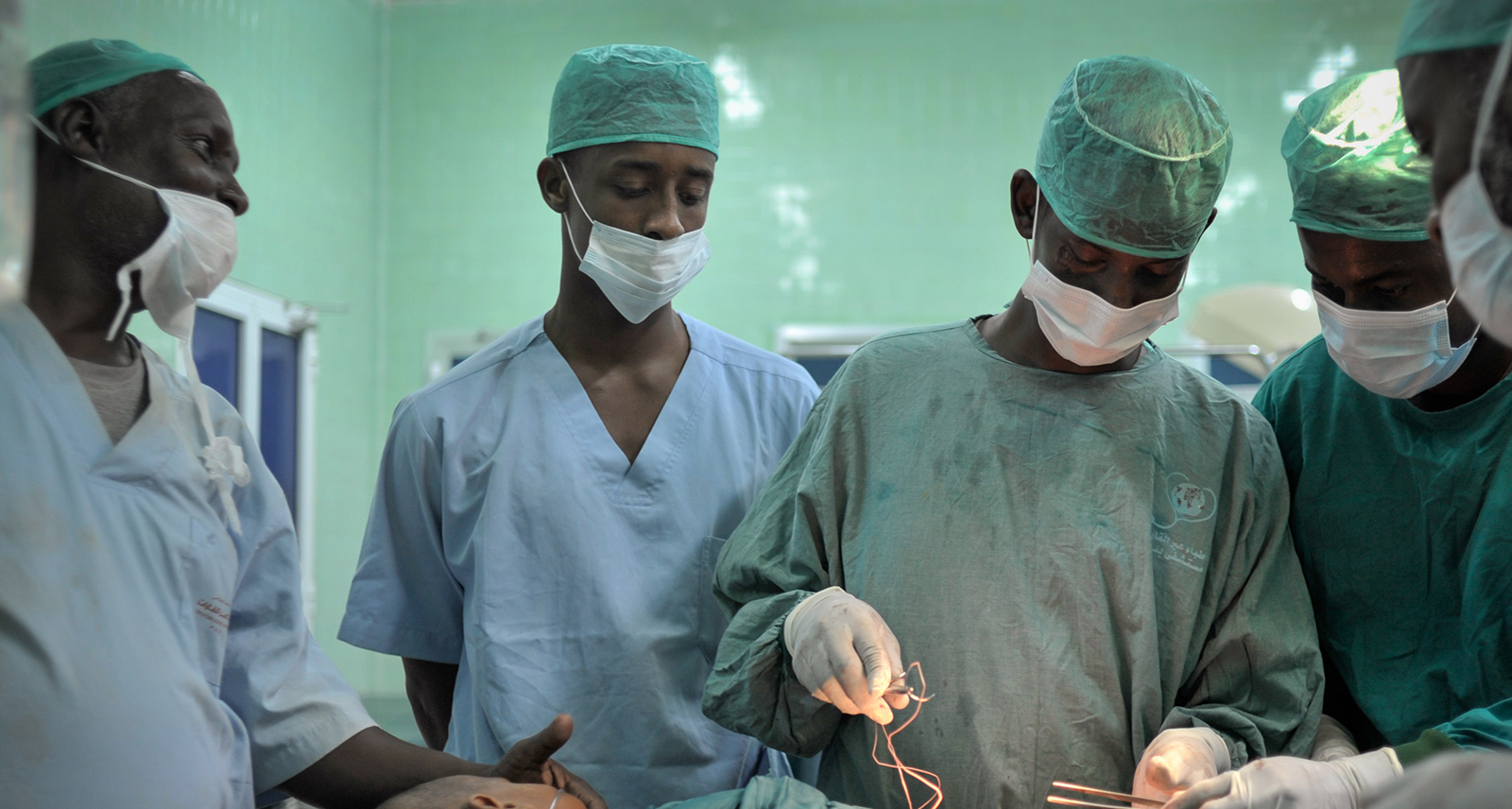
Sepsis is the second biggest cause of death in the world and the leading cause of preventable death. Globally, there are an estimated 30 million cases of sepsis each year, with over 7 million ending in death. Of these deaths, at least 2 million are estimated to occur in Africa. Despite being a major killer, sepsis remains largely unknown by the general public and health care workers, and is under-prioritised by policy-makers.
Sepsis is the 2nd biggest cause of death in the world & the leading cause of preventable death. Despite being a major killer, sepsis remains unknown by general public & health care workers, & is under-prioritised by policymakers. Share on XFrom 14 – 16 June 2019, experts converged in Dar es Salaam under the African Research Collaboration on Sepsis (ARCS) initiative to discuss sepsis in Malawi, Gabon and Uganda and the need to highlight sepsis as a policy issue. The meeting saw experts identify three inter-related problems confronting sepsis in these countries.
First is the need for a standardised definition for sepsis. There are many different definitions of sepsis, even among doctors and experts, and this makes it difficult for most people to fully understand and engage with sepsis. Consequently, there is limited to no population awareness of it. Even amongst medical practitioners, there is only a presumptive diagnosis of sepsis and no point-of-care tests. As a result, practitioners put less emphasis on sepsis but rather look at other diseases associated with it, leading to the second issue of lack of data availability due to the syndromic (and not objective) diagnosis of sepsis. This is compounded by the fact that there is no public budget or private funding for sepsis research in Africa, so it is generally not prioritised. This vicious circle is completed by there being no resources for sepsis-related training or treatment and the third problem: lack of population awareness. There is no word for sepsis in vernacular, and consequently no social chatter in communities about sepsis, which would aid in engaging discussion and building pressure for government intervention. There is also no pressure on the government from the medical profession, who consider it as “small fish” secondary to “real” underlying problems associated with sepsis, such as malaria, TB or HIV.
Based on this, participants embarked on the policy-influencing objective of generating more knowledge to recognise sepsis as a priority disease and put it on the agenda. Specifically, there is a need to converge the problem with policy and politics by engaging with eleven stakeholder groups, namely: Civil Society Organisations, Ministries of Health (MoH), Laboratory personnel, Media, Health recorders, International funders, Researchers, Medical teachers, Clinicians, Ethics committees, and Regulatory bodies.
These stakeholders should be engaged in four low-cost outcome mapping approaches:
- Informing and translating: This policy learning process should target civil society, media, international funders, MoH, medical teachers and regulatory bodies. Various evidence products developed through sepsis research must be disseminated to these stakeholders. For example, the sepsis fact sheet must be disseminated to civil society and media, whereas the sepsis policy brief should be disseminated to MoH and international funders, and curriculum change recommendations to medical teachers and regulatory bodies.
- Linking: This coalition-building process should involve linking sepsis experts to target stakeholders, including MoH technical working groups (TWGs), medical teachers, regulatory bodies and media. Sepsis experts must present to these stakeholders on sepsis-related research through meetings, panel discussions and interviews.
- Matchmaking: This attention-focusing process will bring together ethics committees, clinicians, international funders, allied health workers and researchers. Arrangements should be made for clinical and allied health workers to communicate to ethics committees on the gaps in knowledge to accurately diagnose and report sepsis. Communication between ethics committees and international funders must be facilitated for the latter to speak on the gaps in evidence on sepsis. Finally, communication between ethics committees and researchers can be moderated for the latter to speak on the need for permission to audit patient records to generate the knowledge and evidence on sepsis needed by health workers and international funders.
- Capacity strengthening: This activity should involve training MoH staff on evidence-informed decision making (EIDM). A curriculum developed by the African Institute for Development Policy (AFIDEP) and their partners is a great starting point, and the training delivery can use sepsis as a case study
With sepsis having human and financial costs, these approaches could bring sepsis on the policy agenda, where it needs to be, by converging the problem with policy and politics. Re-shaping the perception of sepsis among key stakeholders and making it a policy issue is vital to reducing cases in Africa, and the world at large. This World Sepsis Day, let us play our part and spread awareness.
https://youtu.be/AEGUCpxwAlE
ARCS is a Global Health Research Group awarded by the National Institute for Health Research (NIHR grant reference number 17/63/42) and led by the Liverpool School of Tropical Medicine (LSTM). This blog presents independent research funded by the NIHR. The views expressed are those of the author and not necessarily those of the NHS, the NIHR or the Department of Health and Social Care.
Related Posts





